“What Is DVT (Deep Thrombophlebitis) ?”
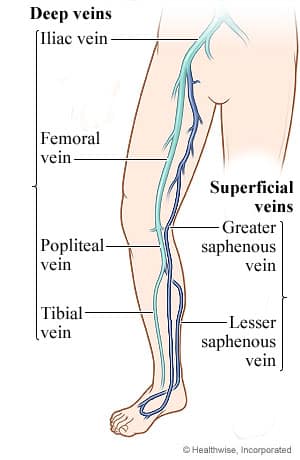
Deep vein thrombosis (DVT) is also referred to in the medical field as deep thrombophlebitis and also referred to as Phlebitis. This is a condition that presents in patients who are suffering from blood clots (thrombus) which are found in the deep veins, most commonly in the legs. Deep veins make up a network of vessels located close to bone and surrounded by dense muscle tissue. These veins are essential for healthy blood flow in the body, as they run further under the skin and return significantly more blood to the heart than surface level, or superficial veins. Learn more about the deep vein thrombosis symptoms below.
DVT Risk Factors
A significant risk factor in the potential development of DVT is the presence of untreated varicose veins. Other risk factors may include but are not limited to: excessive downtime after a surgical procedure, physical trauma, cancer and genetic clotting disorders.
Blood clots occurring alongside inflamed superficial veins create a condition known as superficial deep thrombophlebitis. While this combination rarely causes serious medical issues, a similar scenario occurring in the deep vein network is considered life threatening and should be attended to immediately. Blood clots present a risk in patients as they can potentially dislodge and travel to the lungs, blocking blood flow and causing a pulmonary embolism, which is often fatal. Additionally, risk factors associated with DVT include long-term vein damage and leg sores.
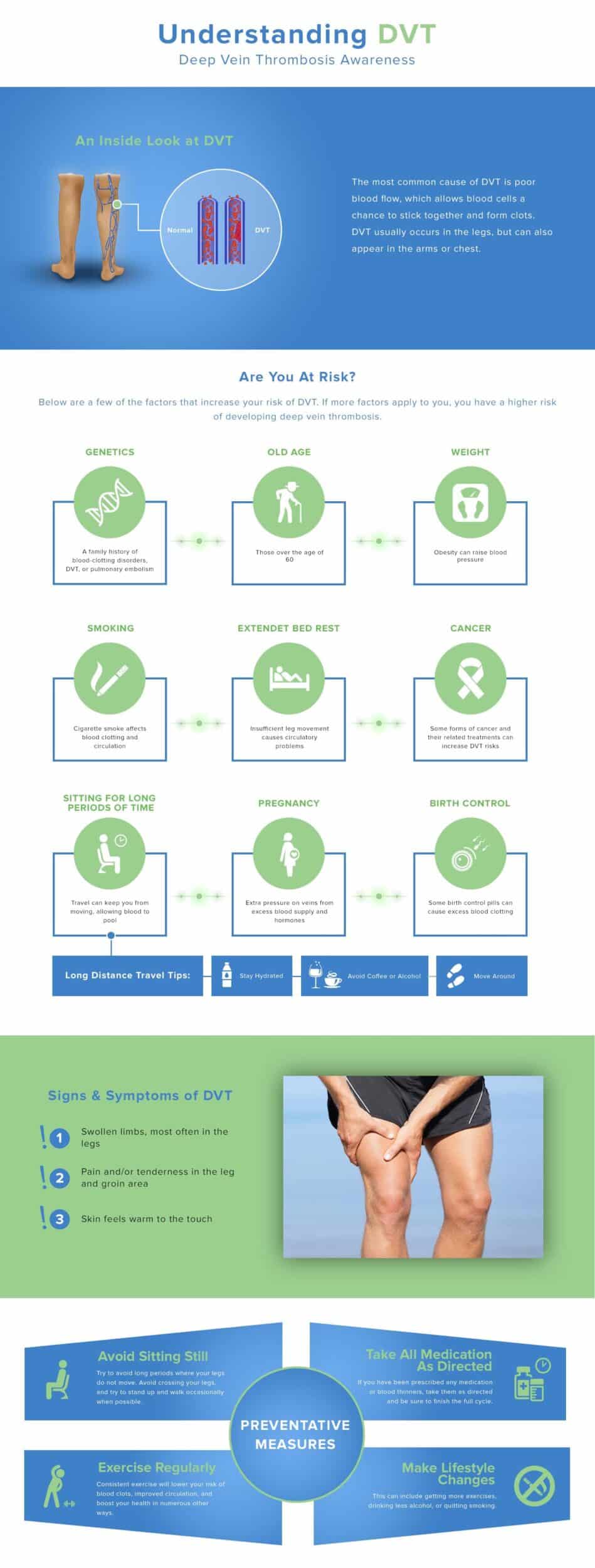
Causes of DVT (Deep Thrombophlebitis)
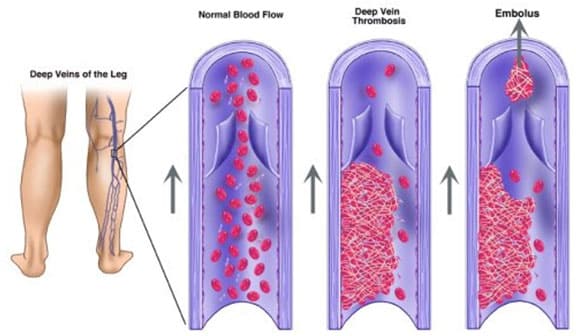
A vein’s inner lining is an essential component to the vein’s overall successful function, and when damage occurs to this area, the potential for a developing blood clot exists. Blood clots form more quickly in individuals who suffer from slow moving blood flow resulting from faulty veins or thicker blood density. For some, blood clots are the inevitable result of a predetermined genetic disorder. Others develop blood clots after extended periods of inactivity which may include bed rest following a medical procedure or situations where a person is required to sit for extended periods of time. Cancer has also been linked to the development of DVT in patients. Varicose veins increase the risk of DVT eightfold over an individual’s life.
Signs and Symptoms of DVT
Deep vein thrombosis presents differently in each patient, but there are a few common symptoms that indicate a person may be suffering from DVT. Symptoms could potentially include swelling of the limbs combined with a warmth and pink or red discoloration. It’s very likely that the calf or thigh may ache and feel tender to the touch.
The greatest risk associated with blood clots is a missed diagnosis. If a blood clot is small, it may not cause any significant symptoms and go completely undetected. Unfortunately for some patients suffering unknowingly from this condition, the occurrence of a pulmonary embolism may be the first and only sign that something was wrong.
Diagnosing DVT
The process of diagnosing DVT is rather simple and can be a life saving opportunity. The attending physician will perform a non-invasive ultrasound of the patient’s veins. A doppler ultrasound test is used to measure the blood flow through veins and identify any clots in real time. Contact Laser Lipo and Vein Center to schedule an appointment if you’re experiencing DVT symptoms.
Treating DVT
It’s imperative that once a diagnosis of DVT is made, treatment begins immediately to reduce the risk of a traveling or growing blood clot. A physician will generally begin with a prescription for a blood thinner such as Heparin or Warfin. While Heparin is delivered by IV injection, Warfin can be consumed in pill form. Patients will then be scheduled for a series of follow-up blood tests so the effectiveness of the medication can be closely monitored and adjusted as needed.
In more extreme cases, a vena cava filter may be recommended to help prevent blood clots from reaching the lungs. This filter is used in the large vein that returns blood to the heart and runs up from both the abdomen and legs. It is highly likely that no matter what course of action is taken concerning treatment, patients will be encouraged to elevate their legs regularly, use a heating pad, incorporate exercise into their daily routines, and wear compression garments. These strategies work to alleviate both pain and swelling.
Deep Vein Thrombosis Symptoms
While the development of DVT cannot be stopped for some patients, there are strategies that can be incorporated into daily life that may slow or reduce their overall risk. Wearing compression stockings, particularly when traveling by air extensively, is highly recommended. Increasing fiber intake aids digestive health and can reduce pressure put on problematic varicose veins. If large varicose veins are present, get them treated. Similarly, increasing Vitamin C consumption can result in greater blood vessel support. Some medical professionals recommend incorporating bioflavonoids into the diet as the antioxidant and anti-inflammatory properties are linked to improved vein-wall health.
Alternating hot and cold baths for legs affected by varicose veins is found by some patients to be an effective strategy for reducing pain and improving overall blood circulation. Additionally, lying horizontally on a bed or couch can be useful in relieving leg pressure.
Deep Vein Thrombosis FAQs
I have a DVT in my left leg and have to wear a compression sock because the valve is broken. Is there a surgical treatment to fix this?
I strongly recommend that you continue to wear the compression stockings per your physician’s recommendation since this has been shown to decrease the chance of “post-thrombotic syndrome.” Additionally, you really need to know which “valve is broken.” A complete ultrasound is needed. If you do not have any DVT anymore and you have superficial venous reflux, that could be treated and you could get an improvement of your symptoms (assuming you have them).