While often an unexpected condition, it’s not uncommon for women to develop varicose veins during the course of their pregnancy. The same hormones that help prepare the body to carry and deliver a newborn also affect primary vein walls. Varicose veins most commonly appear on the legs but can also develop on or near the vulva. Normal weight gain associated with pregnancy results in greater pressure being put on these vessels and can lead to the development of varicose veins in pregnancy. Treating varicose veins during pregnancy is important because, if left untreated, it can only get worse over time. Learn more about treating varicose veins during pregnancy, below.
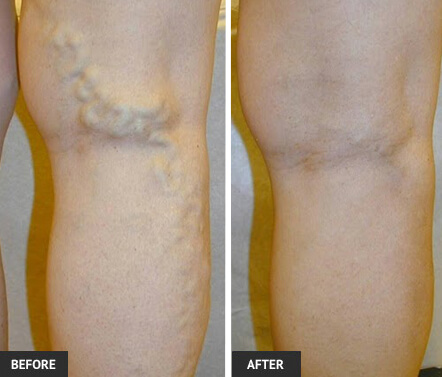
Treating Varicose Veins during Pregnancy in St Louis
Dr. Wright’s results after treating varicose veins during pregnancy are undeniable, check out his before and after pictures.
Varicose Veins
Often appearing on the thighs and legs, varicose veins are enlarged vessels that are associated with unpleasant symptoms for those suffering from the condition. While varicose veins may be considered a cosmetic issue, they are vessels responsible for transferring blood to the heart and are important for overall circulatory health.
Varicose Vein Progression
Unfortunately, women who develop these pregnancy veins will not see the condition disappear once the baby is born. On the contrary, varicose veins have a tendency to worsen over time. The condition is caused by faulty valves in the veins that begin to allow blood to flow backwards, away from the heart, subsequently causing pools to form which distend the vein walls. These valves are unable to heal without medical assistance. Without a proper varicose vein treatment during pregnancy, those with the condition may begin to experience painful symptoms including aching, swelling, tenderness, or restlessness of the legs. The one exception to this is the development of vulvar varicose veins which tend to improve and reduce in appearance once the baby has been delivered.
Factors Affecting Varicose Veins During Pregnancy
Increased estrogen levels during pregnancy are linked to many women developing prenatal varicose veins. Additional factors leading to the development of this condition include obesity, prolonged periods of standing as well as physical trauma that occurs during gestation. Women who carry multiple children to term and develop varicose veins during one pregnancy are more likely to see their condition worsen with each subsequent pregnancy.
Treatment Options for Vulvar Varicose Veins
Options for varicose vein treatment during pregnancy for women who develop vulvar varicose veins are limited, yet fortunately rarely required. Once the baby is delivered, swollen pregnancy veins in this area of the body tend to diminish naturally with very little evidence of their existence remaining long-term. In the event that vulvar varicose veins do not disappear after birth, treatment options similar to those physicians use to treat varicose veins on the legs should be discussed in a professional medical setting.
Treating Varicose Veins During Pregnancy
During a women’s pregnancy, the body naturally gains weight to both cushion the fetus and prepare the body for delivery. While weight gain naturally puts more pressure on vein walls, it is not thought to contribute to the development of varicose veins during pregnancy as significantly as hormones that are released during this time. In the first trimester of pregnancy, women experience an influx of hormones that lead to the relaxation of vein walls. Relaxed walls can ultimately lead to blood reflux and pooling which causes the varicose veins to form.

Questions and Answers:
I had a laser treatment done on a deep vein when I was 4-weeks pregnant and did not know I was. I am now 23-weeks along and am nervous that the use of general anesthesia at such an early time in gestation will cause long term effects.
It is highly recommended that both the mother and fetus be examined by a physician as soon as possible if general anesthesia was used at any point during a pregnancy as this can pose a risk to overall health. At the Laser Lipo and Vein Center, although ablations are not performed during pregnancy, laser ablation is performed exclusively with the use of local anesthesia and if required, a minimal dose of an oral sedative, both of which are entirely safe during pregnancy.
Are there complications during pregnancy after having EVLT? I had this surgery a year ago, then again 4-days ago because the first one was not successful. I would like to get pregnant in the next couple of months, but I’m worried about clots. Should I be, or are there other risks?
While there is no scientific proof linking EVLT to risks during pregnancy, patients who undergo this treatment run a slight risk of developing deep vein thrombosis (DVT) post-procedure. Fortunately, the risk is minimal to non-existent in the several months following the procedure and often times, EVLT will halt the potential for DVT by ablating vein reflux at the source. It is highly recommended that patients with a higher risk for developing DVT regularly wear compression socks to reduce the likelihood of clot development.
While pregnant with my first child I’ve developed a large number of spider veins on my legs/thighs. Are spider veins more prevalent during pregnancy? Do they go away after delivery? Can I get sclerotherapy while I’m pregnant?
While sclerotherapy is a highly effective treatment for many vein conditions, it should not be performed during pregnancy. Instead, women are encouraged to wear compression stockings or support hose during pregnancy as a way to promote blood flow towards the heart and avoid pooling in the legs. Spider veins do tend to appear more rapidly during pregnancy and while some will fade after the baby is born, it is unlikely that they will disappear entirely. After delivery, it is recommended that women wait a short while to see if spider veins developed during gestation fade. In the event the lingering spider veins become a cosmetic issue, sclerotherapy is a viable option to discuss with a physician.