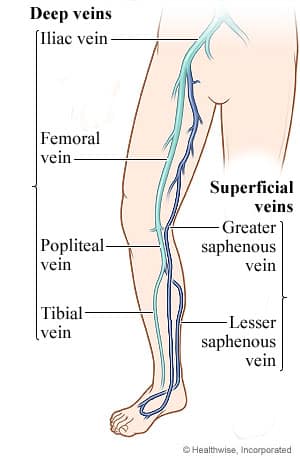
Blood clots that happen in surface veins rarely cause any problems. On the other hand, deep vein clots require immediate medical care due to the danger they present. They can dislodge and move to the lungs and block blood flow. This is known as a pulmonary embolism and can be fatal.
If there is damage to the inner lining of a vein, deep vein clots can form. In addition, if your blood is thicker, or is more likely to clot, deep vein clots may occur. Clots can form if you are inactive. This can include situations where you are bedridden or you sit for long periods of time. Other causes of clots include cancer, injuries or surgery. Heredity and genetics are also known to cause DVT.
Deep vein thrombosis symptoms include swelling, redness, or warmth in the legs. Additionally, the thighs or calves may feel tender or achy. However, should the clot be relatively small, it may not cause any symptoms. Unfortunately, in some cases the first sign of DVT is a pulmonary embolism.
Diagnosis and Treatment of Deep Vein Thrombosis
An ultrasound procedure that measures blood flow is used to identify and diagnose possible clots in the veins.
Should a DVT be identified, immediate treatment is required to prevent the clot from growing or triggering a pulmonary embolism. Treatments usually include Heparin or Warfarin, which are blood thinners. If you are prescribed these medications, you will also undergo regular blood testing to ensure that the drugs are being effective.
Other treatments can involve elevating your legs, exercise, use of a heating pad, and wearing compression socks.
In rare cases, treatments may involve a vena cava filler that will prevent a clot from reaching the lungs.
Preventing Deep Vein Thrombosis
You have several things you can do to help prevent DVT if you feel you are at risk including:
- Increase fiber intake
- Add more Vitamin C to your diet, as it can help maintain healthy blood vessels
- Wear compression socks
- Consider taking a baby aspirin if not contradicted by other health concerns
- Avoid sitting in one place for an extended period of time (more than an hour). Be especially careful when traveling.